Diabetes mellitus, the medical name for “sugar diabetes,” is one of the most common hormone-related (aka endocrine) diseases of dogs. While there’s no cure for diabetes and its management demands your attention daily, proper care can help your dog live a healthy, active life. Read on to learn how nutrition and insulin injections play critical roles in the lives of diabetic dogs.
WHAT IS DIABETES?
Diabetes in dogs is similar to type 1 diabetes in people. It occurs when your dog’s pancreas, an organ of the digestive and endocrine systems, makes too little insulin or stops producing insulin altogether. Diabetes also occurs if your dog’s body tissues don’t respond properly to insulin, a condition known as insulin resistance. The result is a buildup of glucose, a sugar that is the body’s main energy source, in the blood.
INSULIN AFFECTS HOW YOUR DOG’S BODY USES FOOD ENERGY
When your dog eats, some of the carbohydrates in food are broken down into several types of simple sugars, including glucose. Glucose is absorbed from the small intestines into the bloodstream, where it travels through the liver to cells throughout the body.
Insulin is a protein hormone that’s required for glucose to be transferred from the blood into cells where it’s used for energy. If too little insulin is available or cells have an abnormal response to insulin, glucose can’t enter cells. Instead, glucose builds to high levels in the bloodstream, a condition called hyperglycemia.
When glucose can’t enter cells, the cells run out of energy to function normally and they become “starved.” What you might notice at this point is that your dog loses weight despite a ravenous appetite. You might also notice that your dog drinks and urinates more, two classic clinical signs of diabetes. Increased thirst and urination occur because the high level of glucose in the blood has reached a tipping point. The kidneys can no longer recover all of the glucose that is spilling into the urine. Large amounts of water are pulled along with glucose, and together they pass out of the body.
Diabetes is a serious condition that, if left untreated, can:
- Damage the liver, kidneys and/or eyes
- Increase the risk of infections
- Slow the healing of wounds
It can also lead to a life-threatening metabolic condition called diabetic ketoacidosis that requires immediate medical treatment.
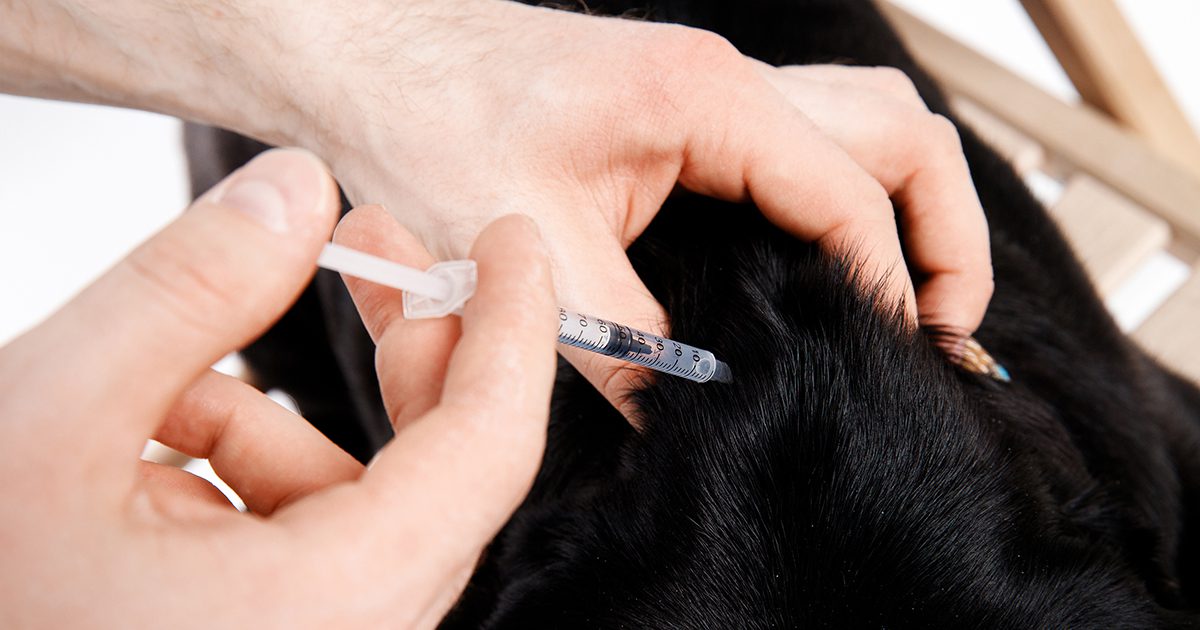
INSULIN THERAPY IS A MUST-HAVE FOR DIABETIC DOGS
Diabetic dogs require lifelong insulin treatment to replace the insulin that their pancreas no longer makes. As with people, no single insulin product effectively manages diabetes in every canine patient, and individual response to insulin therapy can be unpredictable. Veterinarians use a variety of insulin products to help their diabetic patients, often in an extralabel (or “off-label”) manner. As of February 2019, two insulin products are approved by the Food and Drug Administration (FDA) for use in dogs — Boehringer Ingelheim Animal Health’s ProZinc® (protamine zinc recombinant human insulin) and Merck Animal Health’s Vetsulin® (porcine insulin zinc suspension).
ProZinc was only recently approved to treat diabetic dogs, but veterinarians are already familiar with it and have been prescribing it for their canine patients who didn’t respond well to other insulins. A long-acting insulin, ProZinc was first approved for use in diabetic cats in 2009. And although ProZinc is made from recombinant DNA sourced from the human insulin gene, the drug has not been evaluated for use in humans.
CONSISTENCY IS KEY WHEN FEEDING DIABETIC DOGS
Insulin therapy demands that diabetic dogs eat at about the same time as the insulin injection to keep the dog’s blood sugar from dropping too low. Many veterinarians recommend giving the insulin injection just after your dog finishes his or her meal to ensure an appropriate amount of calories (energy) are absorbed.
Ideally, a diabetic dog should be fed two similar meals a day, about 12 hours apart, to avoid unnecessary changes in blood glucose. Insulin is then given within an hour of each meal being eaten, and this schedule should be maintained as consistently as possible.
DIET CAN HELP WITH BLOOD GLUCOSE CONTROL
Some diabetic dogs are very thin while others are overweight or obese. Some may be close to their ideal body weight. A veterinarian will tailor a diabetic dog’s diet to his or her specific body condition and any concurrent health concerns, and will most likely recommend a therapeutic dog food.
The goals of dietary therapy for a diabetic dog are to get the dog to an optimal body weight with appropriate protein and carbohydrate levels, fat restriction, and calorie and portion control. In other words, overweight and obese patients will need to lose weight, while diabetes-associated weight loss must be stopped for those dogs who are underweight.
According to the 2018 AAHA Diabetes Management Guidelines for Dogs and Cats, a diet that corrects obesity, results in optimal body weight and minimizes increased blood sugar levels after eating is recommended. Diabetic dogs can do well with any diet that is complete and balanced, is fed at consistent times in consistent amounts, and is tasty enough that the dog has a predictable and consistent food intake. Many veterinarians recommend feeding a diabetic dog a food that’s high in complex carbohydrates and that contains adequate fiber. Complex carbohydrates increase the amount of time it takes for food to move through the digestive system; fiber delays stomach emptying and absorption of carbohydrates in the small intestine. As a result, glucose is released slowly and evenly into the bloodstream and the post-meal increase in blood glucose is reduced.
Because there are many factors to consider, it’s important to talk to your veterinarian when choosing food for your diabetic dog.
While a diabetes diagnosis for your dog may feel overwhelming initially, diabetes is a condition that you can manage with your veterinarian’s help. Insulin therapy and high-quality nutrition play critical roles in managing your dog’s blood glucose and clinical signs.
RELATED POST: Seven Myths About Pet Diabetes
RELATED POST: Is My Pet at Risk for Diabetes?